Head: prof dr Sven Francque
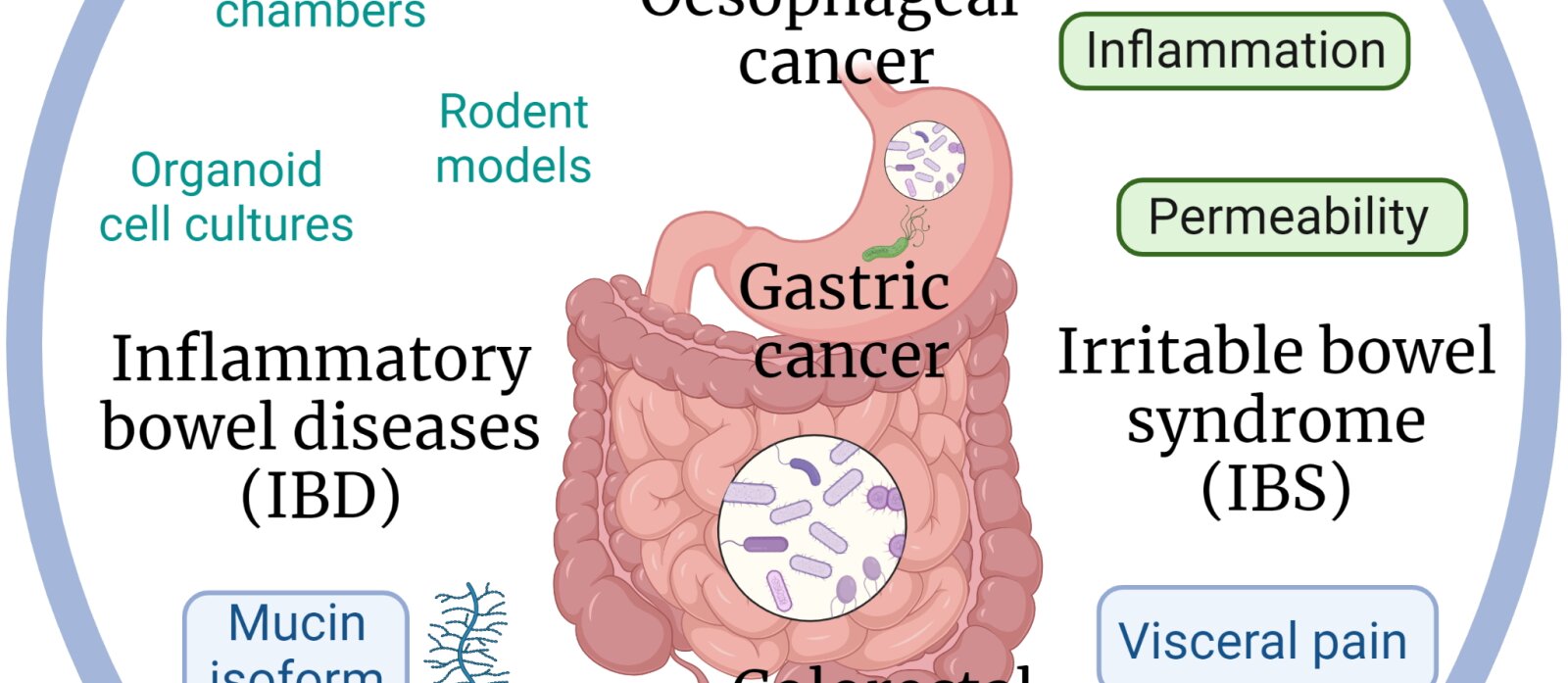
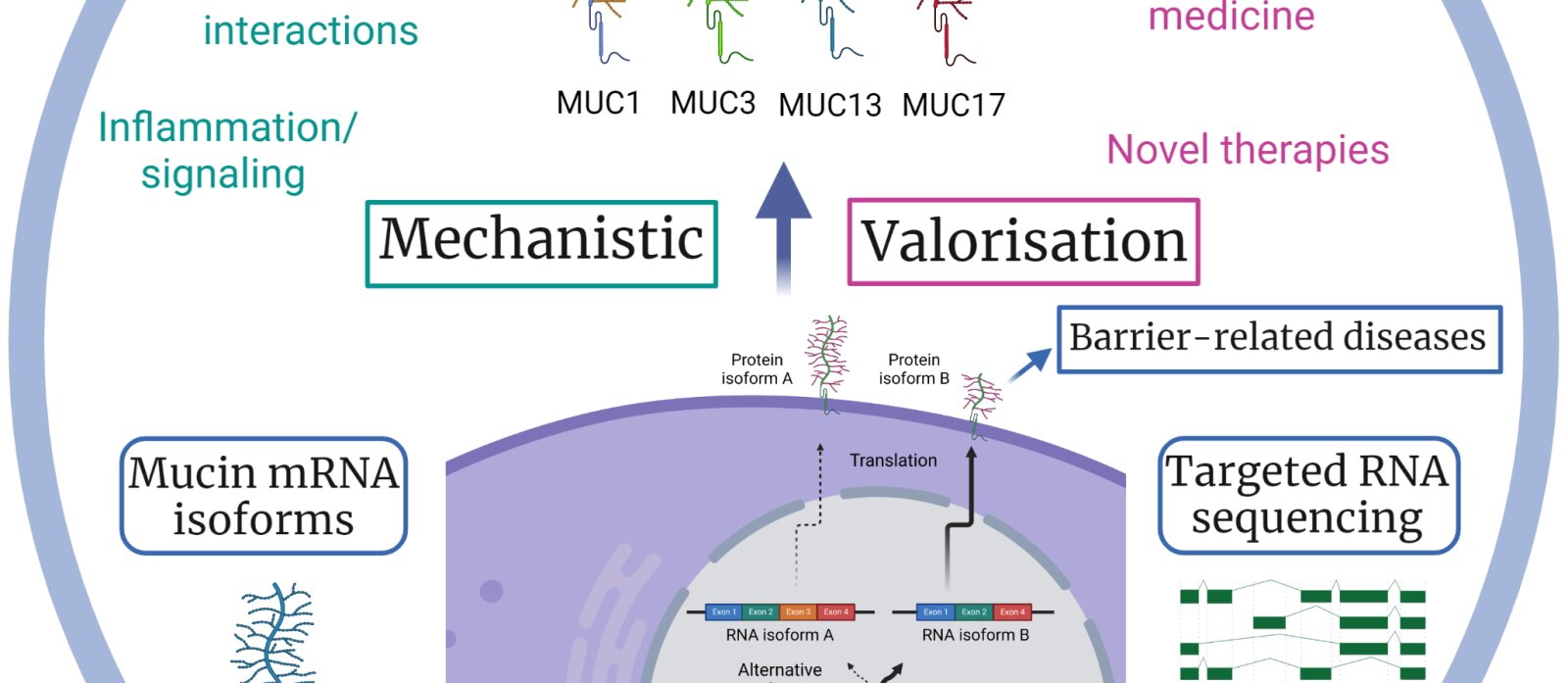
Laboratory of Gastroenterology:
prof dr Benedicte De Winter
prof dr Sven Francque
prof dr Heiko De Schepper
prof dr Sheila Krishnadath
Post docs:
dr Vincent Janmaat
PhD students:
Chen (Benny) Chunting
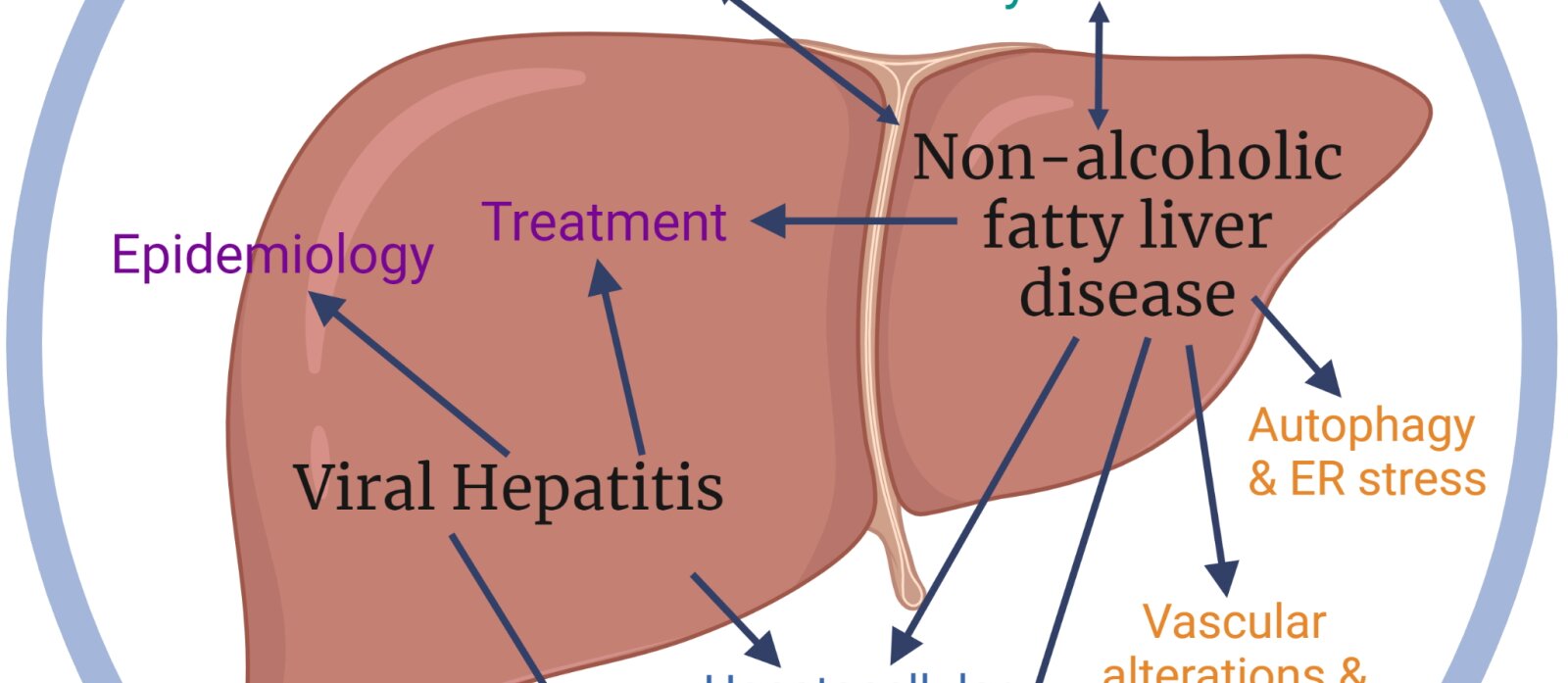
Laboratory of Hepatology:
prof dr Sven Francque
prof dr Thomas Vanwolleghem
Post docs:
dr Tom Adomati
PhD students:
Lotte Schoenmakers
Jonas Weyler