Urology and Urological Rehabilitation
Members
Lab director: Prof. dr. Stefan De Wachter
Research Advisor: Em. Prof. dr. Jean-Jacques Wyndaele, Prof. dr. Lori Birder, Prof. dr. James Gillespie
Research Mission
The animal lab of UROLOGY (part of TNW) focuses on research related to sensory and motor function of the Lower Urinary Tract in small animals.
Special focuses are:
- Bladder – Bowel interaction
- Direct measurement of afferent activity
- Intraurethral mechanical stimulation
- Urethral – Bladder interaction
- Autonomous bladder contractions
- Major Pelvic Ganglion
New projects
- Investigation of urethral sensation
- Peripheral modulation of bladder sensation: motor-sensory system
Investigation of urethral sensation
The focus of this project is the expansion of the knowledge of the urethra, with special attention to the sensations and afferent information that have their origin in the urethra.
In order to function normally, the bladder and urethra need to work together as one unit. This coordinated activity is regulated by a complex neural control system, which incorporates different spinal and supraspinal reflex pathways, where the urethra plays an important role. It has been reported that afferent input from the urethra can modulate bladder function, both in animals and humans.
Though, little is known about the functional properties of urethral afferents. Such knowledge will allow greater insight into the role of urethral afferents in LUT function. In a first study, we identified and described the functional properties of urethral afferents responsive to urethral distention in the female rat [1].
To measure the potentials of urethral afferents, we have used the “single afferent activity (SAA) technique”. This technique has been abundantly used in our laboratory to measure bladder potentials [2-3]. In order to measure urethral afferents, the technique has been modified so that the afferent potentials of both pelvic and pudendal nerve can be measured. This technique will allow the study of urethral afferents under different interventions (distention, flow, drugs). Modulation of urethral afferent/sensory neurons may have a potential role in the treatment of certain pathologies of the LUT, such as stress urinary incontinence and overactive bladder.
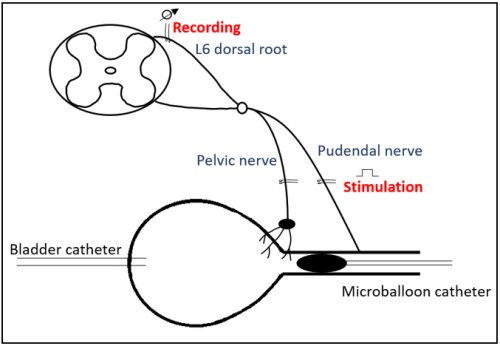
Figure 1: schematic overview protocol of urethral afferent measurements
One needs to keep in mind the possibility of different types of urethral afferents. Different types of immunoreactive nerves have been identified in the bladder of different animals. Next to functional studies, where afferents are solely subdivided by their functional characteristics (current velocity, firing rate, response pattern), structural studies of the urethra are needed to identify the different types of afferents and their locations in the urethra.
So next to functional studies we also developed structural studies of the urethra. The structural studies are developed in collaboration with Professor James Gillespie (Newcastle University). With the use of immunofluorescence we can visualize afferents, muscle and the different morphological layers of the urethra. In a first structural study, we have investigated and characterized the location and distribution of different morphological aspects of the female rat urethra, along its entire length, with particular attention to combine structure and function, in order to gain more knowledge about the overall physiology of the female rat urethra.
A combination of structural and functional studies is essential to an understanding of biological function and to gain more knowledge of normal and pathological conditions in experimental animals, like the rat, and eventually in humans.
References
1. Eggermont M, Wyndaele JJ, Gillespie J, De Wachter S. Response properties of urethral distension evoked unifiber afferent potentials in the lower urinary tract. J Urol, article in press
2. Aizawa N, Igawa Y, Nishizawa O, Wyndaele JJ. Effects of CL316,243, a beta 3-adrenoceptor agonist, and intravesical prostaglandin E2 on the primary bladder afferent activity of the rat. Neurourology and urodynamics. 2010 Jun; 29(5): 771-6.
3. Minagawa T, Wyndaele M, Aizawa N, Igawa Y, Wyndaele JJ. Mechanisms of pelvic organ cross-talk: 2. Impact of colorectal distention on afferent nerve activity of the rat bladder. The Journal of urology. 2013 sep; 190(3): 1123-30.
Peripheral modulation of bladder sensation: motor-sensory system
The bladder is not quiescent during the urine storage phase. Non-voiding bladder contractions that increase in amplitude and frequency have been observed during bladder filling. The exact role or purpose of non-voiding contractions is still unknown, but they are thought to be able to induce afferent activity and therefore serve as a primary sensory mechanism within the lower urinary tract. Enhancement of this activity might then result in the development of overactive bladder (OAB) syndrome, a highly prevalent disorder estimated to affect 50–100 million people worldwide and characterized by symptoms of urgency, urinary frequency and nocturia, with or without urgency incontinence.
Non-voiding contractions can also be observed in vitro using an isolated whole bladder preparation oxygenated in an organ bath. Measurements of this autonomous activity in an isolated rat and guinea pig bladder are performed in our lab to evaluate the intrinsic control mechanisms residing in the bladder wall that are responsible for the generation and modulation of non-voiding activity. The assessment of the control pathways involving non-voiding activity is further expanded using an in vivo rat model. The influence of the central and peripheral nervous system on non-voiding activity is analysed using a transection protocol, developed in our lab, in which NVA is evaluated before and after transecting the hypogastric nerves, pelvic nerves and the major pelvic ganglia. An important role for the major pelvic ganglia in the modulation of NVA has been observed. /Poster dept_Urology.pdf (Download poster)
The use of a rat model with a partial obstructed bladder, which is frequently used to study OAB, will further elucidate the importance of local reflexes in the major pelvic ganglion for the generation of NVA during pathology. Furthermore, the impact of β3-adrenergic drugs on these local reflexes will be determined.
These studies are developed in collaboration with Professor James Gillespie (Newcastle University). Via an immunohistochemistry technique developed in Newcastle, we are able to map the structural components inside the bladder wall and the major pelvic ganglion that might be involved in our functional observations.
These studies will contribute to a better understanding of the clinical problems associated with OAB and the (patho)physiological mechanisms of non-voiding activity and bladder sensation.